About This Article: Zoom Health has supplied home health tests to UK customers for nearly 20 years. This guide draws on our experience helping thousands of people monitor their health and understand high blood pressure. Always consult a healthcare professional for medical advice.
Published: 28 December 2023 | Last Updated: 16 February 2026 | By: Anthony Cunningham
In This Article
- Understanding the Global Rise in High Blood Pressure
- The Increasing Burden on Developing Nations
- The Importance of Prevention and Control Measures
- The Gender Gap in Hypertension
- How Nations Compare on High Blood Pressure
- Promising Progress in Some Developing Nations
- Improving Hypertension Detection Through Screening
- Monitoring Your Blood Pressure at Home
- Global Solutions to Address the Epidemic
Understanding the Global Rise in High Blood Pressure
Several factors have driven the global rise in high blood pressure since the 1970s. The overall growth and ageing of the world’s population means there are simply more people at risk. However, the study indicates lifestyle changes relating to diet and exercise in developing nations are fuelling the epidemic. As countries become more prosperous, diets get richer in sugars, refined carbohydrates and unhealthy fats, while physical activity declines. This fuels surges in associated health risks like obesity and diabetes.
People in developing countries often have limited access to screening and treatment for high blood pressure. This means many are living with undiagnosed and uncontrolled hypertension, further elevating their risk of heart disease and stroke. The World Health Organization estimates that hypertension now affects 1.4 billion adults worldwide and remains a major cause of premature death.
According to the NHS, high blood pressure often has no symptoms, which is why many people live with it for years without realising. Regular monitoring is the only reliable way to detect it early.
The Increasing Burden on Developing Nations
While blood pressure rates have fallen in many high-income countries, developing regions have seen stark increases. The study found the largest rises occurred in South Asia and Sub-Saharan Africa. In South Asian countries like Bangladesh and Nepal, age-standardised high blood pressure rates rose from 17% to 24% in men and 13% to 18% in women between 1975 and 2015. Rates also approximately doubled in Ethiopia and Malawi over the 40-year period.
Researchers said the worst-affected areas often faced a “triple whammy” of inadequate medical treatment, poor nutrition, and high salt intake. Addressing these factors with policy initiatives should be an urgent priority. As Professor Majid Ezzati from Imperial College London emphasised, profound changes in diet and lifestyle have seen blood pressure rise sharply in low- and middle-income countries, and resources must be mobilised to help them respond.
The WHO’s 2023 Global Report on Hypertension reinforced these findings, noting that two-thirds of adults with hypertension now live in low- and middle-income countries. The report called it a “race against a silent killer” and urged governments worldwide to take action.
The Importance of Prevention and Control Measures
The NCD-RisC study published in The Lancet highlights the critical role government public health policies play in shaping hypertension trends. It found the most impressive reductions in population blood pressure occurred in high-income countries like Canada, the United Kingdom, Australia, and the United States. For example, age-standardised hypertension rates declined from 38% to 24% in Canadian men and 26% to 17% in Canadian women.
These wealthy Western nations have generally had more success promoting healthier diets, implementing salt reduction programmes, and improving access to blood pressure screening and medications. The UK in particular has been leading the charge on salt reduction by setting voluntary sodium targets for the food industry. This comprehensive public health approach serves as a model for tackling hypertension globally.
The British Heart Foundation recommends that all adults should have their blood pressure checked regularly, particularly those over 40. Early detection through routine screening is one of the most effective ways to reduce the risk of heart attack and stroke.
The Gender Gap in Hypertension
The study found that men tend to have higher blood pressure than women across most world regions. There are several potential reasons behind this gender gap.
Biological differences may make men intrinsically more susceptible to hypertension. Hormonal factors are thought to offer some protection for premenopausal women. Lifestyle risks like smoking, heavy alcohol intake, and poor diet quality also tend to be higher in men, contributing to greater cardiovascular disease risk overall.
Men can also have poorer adherence to medications and tend to visit doctors less frequently. This may result in worse blood pressure control over time. Understanding and addressing the drivers of gender disparities in hypertension control should form part of national public health initiatives.
How Nations Compare on High Blood Pressure
The study included blood pressure data from 154 countries, providing insights into how the hypertension burden varies by region.
The countries with the lowest blood pressure averages were South Korea and Canada, with 2015 systolic blood pressure around 118mmHg for men and 111mmHg for women. The highest average blood pressures were in Slovenia for men (138mmHg) and Niger for women (133mmHg systolic).
Europe demonstrated significant regional variations. The UK, Ireland and Nordic countries like Sweden had some of Europe’s lowest rates. Meanwhile, Central and Eastern European nations including Slovenia, Lithuania and Croatia continued to have highly elevated blood pressure averages.
Oceania, North America and Western Europe mostly had lower hypertension rates compared to other regions, though French Polynesia and Greenland stood out for having high blood pressure averages. Latin American countries spanned the spectrum, with Peru and Ecuador having low averages and Paraguay and Bolivia having high rates.
In Africa, blood pressure levels differed starkly between the north and Sub-Saharan regions. Mauritania, Morocco and Ethiopia registered concerning increases. For Asia, South Korea, Singapore and Nepal were among the lowest, while several Central Asian countries like Mongolia and Kazakhstan had very high averages.
These regional comparisons demonstrate the complexity of addressing hypertension but also reinforce that public health policies can lower population blood pressure. While the problem has grown worldwide, declines in Western countries provide a hopeful note.
Promising Progress in Some Developing Nations
While the overall trend is concerning, a few developing countries have managed to reduce high blood pressure rates through concerted efforts.
Costa Rica experienced a decline from around 57% to 21% for men and 44% to 11% for women between 1975 and 2015. The country undertook nationwide initiatives to reduce dietary salt, increase fruit and vegetable intake, and improve access to primary healthcare.
Chile also saw reductions over 40 years, attributed to progressive public health policies improving risk factors like obesity. However, its blood pressure levels remain higher than in Costa Rica. Cuba experienced a remarkable decline from 43% to 32% among men and 37% to 22% in women over the period. Its model of universal health coverage and population health focus has likely supported hypertension progress.
These examples demonstrate that with sustained commitment, developing countries can curb hypertension rates even with limited resources.
Improving Hypertension Detection Through Screening
In addition to government prevention policies, increased screening has an important role in tackling high blood pressure globally. In 2017, 2018 and 2019, the International Society of Hypertension coordinated an awareness and screening initiative called May Measurement Month (MMM). It involved volunteers offering free blood pressure tests around the world during May.
The massive screening drive tested over 4.2 million adults across nearly 100 countries over three years. It identified almost one million people with previously undiagnosed or inadequately controlled high blood pressure. This highlights the value of community outreach programmes in detecting hypertension and connecting people to lifesaving treatment.
In the UK, the NHS offers free blood pressure checks at many pharmacies for people aged 40 and over. Adults in England aged 40 to 74 without pre-existing conditions are also entitled to a free NHS Health Check every five years, which includes a blood pressure assessment.
Monitoring Your Blood Pressure at Home
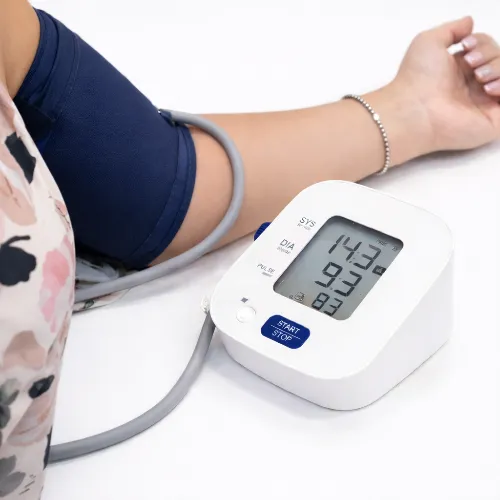
While global efforts focus on large-scale screening, individuals can take a proactive step by monitoring their blood pressure at home. Home monitoring gives you and your doctor a more complete picture of your blood pressure throughout the day, rather than relying solely on occasional readings at the surgery.
Home readings can help detect “white coat syndrome,” where blood pressure appears higher at the doctor’s due to anxiety, or “masked hypertension,” where readings are normal at the clinic but elevated at home. The NICE guidelines on hypertension recommend home monitoring as part of confirming a diagnosis and managing treatment.
For accurate results, it is important to use a clinically validated upper arm monitor. Sit quietly for five minutes before taking a reading, keep your arm supported at heart level, and take two readings one to two minutes apart. Recording your results over several days gives a much clearer picture than a single measurement. You can learn more about correct technique in our guide on how to read blood pressure monitor results.
Take Action: The Kinetik Wellbeing Automatic Blood Pressure Monitor (WBP1) is clinically validated by the British and Irish Hypertension Society. With one-button operation, 90-reading memory, and irregular heartbeat detection, it makes accurate home monitoring simple. The adjustable cuff fits arm circumferences from 22–42cm.
What Customers Say
★★★★★ Taff – March 2020
“Unit arrived quickly and well packed. Once unpacked and working I found the unit easy to use and it stores away nicely in the pouch that comes in the box. Good for recording blood pressure and pulse readings for my regular trips to the GP.”
★★★★★ Dale – March 2020
“Great little machine – I use it to monitor daily changes in my blood pressure and it works well. Recommended.”
★★★★★ Gillian – March 2020
“This small gadget is great. I’ve found that its readings are as accurate as the larger blood pressure monitor I have at my office. It’s nice and portable which is the bonus for me.”
Global Solutions to Address the Epidemic
The shifts in hypertension prevalence underscore it is no longer a condition confined to wealthier nations but one requiring urgent action worldwide. As the NCD-RisC study authors emphasised, solutions must focus on supporting poorer nations to implement evidence-based policies.
Strategies should include national dietary changes to reduce salt, sugar and unhealthy fats; improving produce affordability and accessibility; and health system strengthening to detect and control high blood pressure effectively. With diligent application of prevention and treatment approaches, even hard-hit developing countries can hope to reverse rising blood pressure rates.
The epidemic growth of hypertension globally is undoubtedly alarming. Yet successes in bringing down population blood pressure in some Western nations demonstrate it is possible. Implementing policies today to equip developing countries to confront hypertension can help stem a growing health crisis. On a personal level, knowing your numbers through regular blood pressure monitoring remains one of the simplest and most effective steps you can take to protect your cardiovascular health.
About the Author
Anthony Cunningham – Health Writer & Editor
Anthony Cunningham, BA (Hons), MA, is a UK-based health writer and editor with over 20 years’ experience running Zoom Health, a trusted source for home health tests, preventive care, and wellness guidance. He creates clear, evidence-based articles using NHS, NICE, and WHO guidance. Where possible, content is reviewed by practising clinicians to enhance accuracy and reliability, helping readers make informed healthcare decisions.
You May Also Like
Explore more articles on blood pressure and heart health:
- Home Blood Pressure Monitoring Guide
- Reducing Stress to Lower High Blood Pressure
- How to Properly Use a Wrist Blood Pressure Monitor