Irritable Bowel Syndrome (IBS) is a common gastrointestinal disorder affecting the stomach and intestines. It causes chronic symptoms like abdominal cramps, bloating, and irregular bowel habits. While lifestyle changes can help mild cases, medication and counselling provide relief for more severe IBS.
Understanding IBS
IBS disrupts the digestive system due to increased nerve sensitivity in the gastrointestinal tract. Research indicates this hypersensitivity triggers various discomforts, stemming from complex nerve-brain communication problems.
In the UK, IBS prevalence is estimated between 10-20% of the population. Symptoms often start between ages 20-30, becoming less likely after 40. However, other health conditions of the bowel, causing similar symptoms, become more common after 40. Remarkably, women are twice as likely as men to report IBS symptoms.
IBS is different from inflammatory bowel disease (IBD). This distinction is important given their distinct characteristics and implications. In this comparison, IBS doesn’t involve structural bowel changes or increased colorectal cancer risk.
Recognising IBS Symptoms
IBS entails persistent symptoms commonly including abdominal pain, cramps, bloating, and altered bowel patterns leading to discomfort and distress.
Primary Indicators:
- Abdominal Pain and Cramps: Often in the lower abdomen, particularly after meals and bowel movements.
- Altered Bowel Habits: Changes in frequency, consistency, and appearance of bowel movements, sometimes with mucus.
- Bloating: A sense of fullness and swelling, fluctuating during the day with potential relief after bowel movements.
Triggers and Associated Symptoms:
- Stress: Symptoms can worsen during stressful periods.
- Dietary Influence: Certain foods like fatty or gas-producing items may aggravate symptoms.
- Additional Effects: IBS can cause tiredness, nausea, bladder problems , indigestion, backaches, headaches, and bladder problems.
Differentiating from Similar Conditions:
- Inflammatory Bowel Disease (IBD): Careful diagnosis is needed to distinguish IBS from IBD conditions like Crohn’s and colitis.
- When to Seek Medical Aid: Persistent symptoms warrant consulting a GP. New symptoms after 40 or concerning signs like bleeding or weight loss require prompt medical attention as they could indicate serious underlying problems.
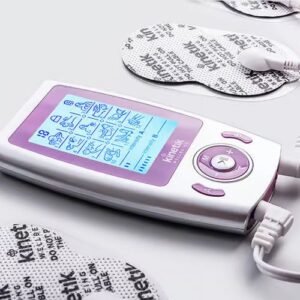
Kinetik Wellbeing Dual Channel TENS Machine TD3
Using TENS Therapy for IBS
Transcutaneous Electrical Nerve Stimulation (TENS) is emerging as an innovative solution for managing IBS and constipation. TENS units work by delivering low voltage electrical impulses through electrodes placed on the skin. This stimulates nerves and muscles, providing therapeutic effects.
TENS devices are designed to intercept pain signals travelling to the brain. By temporarily blocking these transmissions, TENS units effectively relieve muscle spasms and discomfort. This makes TENS a trusted choice for various conditions like back pain.
Experts now highlight TENS potential for addressing IBS and constipation concerns. Strategically placing electrodes on the abdomen and lower back has demonstrated promising results. Ongoing research is uncovering optimal TENS configurations for managing these digestive issues.
How TENS Therapy Works
TENS units send electrical impulses through the skin that stimulate nerve fibres. This stimulation triggers the release of the body’s natural painkillers, called endorphins. Endorphins block pain signals from reaching the brain, providing pain relief.
For IBS, TENS therapy can help relax intestinal muscles and stimulate motility to relieve abdominal pain, cramps, and constipation. The gentle electrical signals may also help reduce inflammation in the digestive tract.
TENS therapy offers a non-invasive, drug-free approach to managing IBS discomforts. It provides temporary relief while being used and can be combined with other treatments. Patients can self-administer TENS at home as needed for pain episodes.
Using TENS Units Effectively
Follow these tips when using TENS therapy for IBS or constipation:
- Switch the unit off before attaching electrodes to skin. Avoid irritated areas.
- Don’t place electrodes on mucous membranes. Consider shaving hair to prevent skin tugging.
- Activate the unit after securing electrodes. Adjust stimulation to a comfortable tingling sensation.
- Typical sessions last 20-30 minutes. Use the device multiple times daily if needed.
- For IBS and constipation, place two electrodes on each side of the lower abdomen and two more on the lower back. This maximizes effectiveness.
- Replace electrodes monthly if using regularly, as the conductive gel wears down over time. Opt for self-adhesive or sensitive skin electrodes for easier use.
Additional IBS Management Strategies
Living symptom-free is the main goal when treating IBS. Approaches range from stress management to dietary and lifestyle changes.
- Lifestyle Adjustments: Stress control, trigger food avoidance, exercise, hydration, and sufficient sleep.
- Dietary Modifications: Eliminating gas-producing foods, gluten, or FODMAP carbohydrates can provide relief for some. Seek dietitian guidance.
- Counselling: Recommended for moderate/severe cases, especially if stress or depression are factors.
- Medications: Fiber supplements, laxatives, anti-diarrheals, and medications like Lyrica or Neurontin can be helpful.
In summary, TENS therapy is emerging as an innovative approach for managing IBS and constipation symptoms. Using these electric nerve stimulation devices, along with other lifestyle strategies, offers a promising route to lasting relief.
Photo “IBS Woman” by Anthony Cunningham for Zoom Health
Zoom Health is a leading UK supplier of Home Health Tests and Earplugs





